Introduction
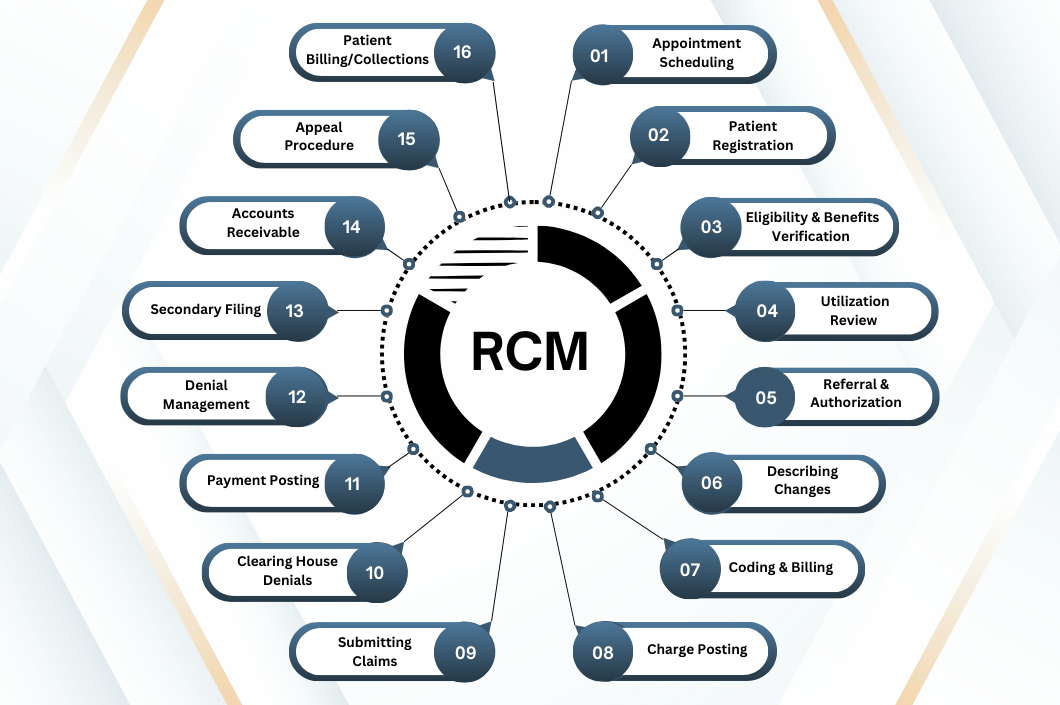
Revenue Cycle Management (RCM) is the cornerstone of financial stability and operational efficiency for healthcare organizations. It encompasses everything from the moment a patient schedules an appointment. The process continues until the healthcare provider receives the final payment for services rendered. Understanding and optimizing each step within the RCM workflow not only maximizes revenue, but also improves patient satisfaction, reduces administrative burden, and ensures compliance with healthcare regulations.
Patient Scheduling and Pre-Registration
The RCM journey starts with patient scheduling and pre-registration. When a patient calls or uses an online portal to book a visit, the front-office staff capture initial demographic information. They also record basic insurance details. Pre-registration ensures that subsequent steps like insurance verification and billing progress smoothly by laying the foundation for accurate data collection. This step is essential for reducing wait times and eliminating repeated requests for patient information.
Registration and Insurance Verification
Upon arrival at the healthcare facility, patients undergo the registration process. Staff formally check in the patient, updating and verifying all demographic and insurance details. Insurance verification is performed, checking eligibility, determining coverage, and identifying co-pays or deductibles upfront. These activities minimize downstream claim denials and help patients understand their costs before services are provided.
Authorization and Referrals
For procedures that require insurance authorization, the provider submits the necessary documentation to obtain approval from the payer before treatment is delivered. In the Revenue Cycle Management workflow, missing prior authorization is one of the most common causes of Claim Denials, making this step a critical component in maintaining clean claims and steady cash flow. Additionally, if specialist referrals are required, the administrative team ensures all referral documentation is processed accurately to avoid disruptions in the RCM process.
Service Delivery and Documentation
As care is administered, providers and support staff meticulously document every service provided, including procedures, treatments, medications, and supplies. Accurate clinical documentation is the bridge connecting patient care with revenue. It justifies the claims submitted and supports medical necessity during payer audits. Comprehensive and timely documentation is integral for correct billing and reducing audit risks.
Charge Capture
Charge capture is the process of recording all billable services rendered to the patient, and it plays a vital role in the overall Revenue Cycle Management workflow. Healthcare providers use secure electronic medical record (EMR) systems to enter charges immediately after providing care. This step is crucial for ensuring that no service or supply is overlooked when preparing claim submissions, which directly impacts accurate reimbursement and financial integrity.
Medical Coding
Medical coders review the clinical documentation and translate encounters, diagnoses, and procedures into standardized codes, such as ICD, CPT, and HCPCS. Coding accuracy is paramount since errors can lead to billing for services at the wrong level, resulting in lost revenue or compliance issues. Regular coder training and technology-driven coding solutions help minimize mistakes and stay aligned with changing guidelines.
Claims Creation and Submission
Once charges are captured and coded, claims are prepared for submission to payers. Electronic claim submission is preferred for its speed and reliability. Clearinghouses and claim management platforms automatically check for errors or missing data, reducing rejections and delays. Timely and error-free claim submission prevents interruptions in cash flow and helps providers receive payments swiftly.
Payment Posting and Reconciliation
After claims are processed by the payer (insurance company), payments and explanations of benefits (EOBs) are posted to the correct patient accounts. This stage involves reconciling payments against billed amounts, identifying underpayments, and resolving any discrepancies. Automated payment posting systems speed up the process and improve accuracy, while staff regularly review outstanding balances to prevent missed revenue.
Denial Management
Despite best efforts in front-end processes, some claims are inevitably denied. The denial management stage involves identifying the root causes of denials such as documentation errors, missing authorizations, or coding issues and correcting and resubmitting claims as needed. Healthcare organizations that invest in robust denial management succeed in recovering lost revenue and refining their workflows for future claims.
Patient Billing and Collections
Once insurance payments are received, providers bill patients for any remaining responsibility, such as co-pays, deductibles, or services not covered by insurance. Patient statements and invoices should be clear, accurate, and provide easy payment options. Providers may offer online payments, payment plans, or work with third-party agencies to collect outstanding balances. Effective patient billing processes reduce bad debt and improve cash flow.
Reporting, Analytics, and Continuous Improvement
The final phase of Revenue Cycle Management, but one that never truly ends, involves tracking key performance indicators (KPIs) and analyzing workflow efficiency. Common RCM metrics include days in accounts receivable, denial rates, net collection percentage, and patient satisfaction scores. Modern RCM systems feature real-time dashboards and automated analytics. These tools enable healthcare leaders to spot trends, optimize processes, and achieve revenue goals..
Conclusion
The Revenue Cycle Management workflow is the financial backbone of healthcare. From patient check-in to final payment, every step requires accuracy, compliance, and coordination. Errors in even one stage can result in denied claims, revenue leakage, and dissatisfied patients.
By partnering with experts like Alpine Pro Health, providers can streamline the RCM workflow, enhance compliance, and maximize reimbursement. With our end-to-end RCM services, we help healthcare organizations achieve both financial health and operational excellence, so they can focus on what matters most delivering quality patient care.